For a broader understanding of how this fits into recovery strategies, see:
What Actually Happens During Wound Healing
Wound healing follows a structured biological sequence:
- Inflammation – immune cells move to the injury site
- Proliferation – tissue begins rebuilding through cell growth and angiogenesis
- Remodelling – tissue strengthens and reorganises
This process depends on several key factors:
- Blood flow and oxygen delivery
- Cell migration and proliferation
- Collagen formation and tissue strength
If any of these stages are disrupted, common in high physical stress environments like sport, healing may slow or stall.
Where Magnetic Fields Fit Into the Healing Process
Magnetic field therapy is considered a biophysical intervention, meaning it interacts with the body’s natural processes rather than replacing them.
Research suggests static magnetic fields (SMFs) may influence:
- Cell behaviour and migration
- Inflammatory responses
- Microcirculation and blood flow
- Collagen formation and tissue strength
For example:
- SMFs have been reported to enhance cell proliferation and migration, both essential for tissue repair
- They may influence vascular tone and blood flow, which supports nutrient delivery to injured tissue
Importantly, these effects are still being studied, and outcomes can vary depending on field strength, application, and biological context.
What Experimental Studies Show About Healing Speed
One controlled study using a static magnetic field applied over wounds found:
- Average healing time reduced to 15.3 days
- Compared to 20+ days in control groups
This represents a ~25–27% faster healing rate under those experimental conditions.
Other animal studies report:
- Faster wound closure rates
- Increased tissue strength
- Improved collagen deposition
In diabetic wound models (where healing is typically impaired), SMF exposure has been observed to:
- Accelerate closure
- Improve revascularisation
- Enhance tissue regeneration markers
These findings suggest a potential supportive role for magnetic fields in recovery environments where healing is compromised or delayed.
A Relatable Scenario: Returning to Training After Skin Injury
Imagine an athlete recovering from a deep abrasion or post-surgical incision.
Even once the wound appears closed:
- Tissue strength may still be reduced
- Inflammation may persist beneath the surface
- Reinjury risk remains elevated
Research indicates that magnetic fields may influence:
- Granulation tissue formation
- Microvascular development
- Inflammatory balance
These are all factors that matter not just for healing but for returning to full training safely.
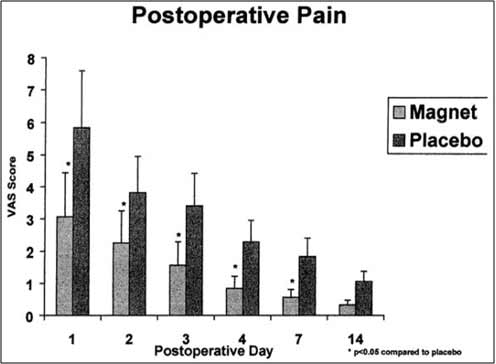

Positioning of magnets in Cepeda study around the surgical incision. Any wonder there was no effect!
Practical Application (Field | Dose | Placement)
In real-world use, outcomes depend on how magnetic fields are applied.
Field
Static magnetic fields used in studies range from low to moderate intensity, often designed to interact with tissue without invasive methods
Dose
Studies vary widely (from ~23 gauss to hundreds of mT), and optimal dosing is not yet standardised.
Placement
In experimental models, magnets are typically placed:
- Directly over the wound
- On top of a dressing layer
- In continuous contact during healing
For a deeper breakdown of application principles:
What the Evidence Does and Doesn’t Say
While results are promising, there are important limitations:
- Many studies are animal-based, not human clinical trials
- Evidence across studies is inconsistent and sometimes conflicting
- Mechanisms are not fully understood
Even the primary study notes that:
- High-quality clinical trials are lacking and difficult to conduct
- The role of magnetic therapy in practice is not yet conclusively defined
This means magnetic fields should be viewed as a potential supportive tool, not a standalone solution.
Where This Fits in Athlete Recovery
For athletes, the relevance is clear:
- Faster tissue repair may reduce downtime
- Improved tissue quality may reduce reinjury risk
- Non-invasive approaches are easier to integrate into recovery routines
Magnetic field exposure has been explored as an adjunct approach, working alongside standard recovery strategies, not replacing them.
Practical Takeaway
Magnetic fields may influence wound healing by interacting with:
- Cellular repair processes
- Blood flow and inflammation
- Tissue regeneration pathways
However:
- Results vary
- Evidence is still developing
- Application matters
Next Steps
If you’re exploring recovery tools that support healing:
- Learn how magnets are used in broader recovery strategies → magnetic therapy for sports injury recovery
- Understand correct application → field, dose, and placement
- See how this fits into injury recovery → sports injury recovery
Magnetic field applications are being studied as one such tool but should be used thoughtfully within a broader recovery plan.
References
Aliabadi, A., et al. (2012). “Evaluation of the effect of static magnetic field in treatment of tendon injuries in dog.” DOI
Cepeda, M., et al. (2007). “Static magnetic therapy does not decrease pain or opioid requirements: A randomized double-blind trial.” PMID: 17242082; DOI
Ebrahimdamavandi, S., et al. (2019). “Application of a static magnetic field as a complementary aid to healing in an in vitro wound model.” PMID: 30625046
Eccles, N.K., et al. (2005). “A pilot study to determine whether a static magnetic device can promote chronic leg ulcer healing.” PMID: 15739653; DOI
Jaberi, et al. (2011). “A moderate-intensity static magnetic field enhances repair of cartilage damage in rabbits.” PMID: 21820604; DOI
Jing, D., et al. (2010). “Effects of 180 mT static magnetic fields on diabetic wound healing in rats.” DOI
Jing, Z., et al. (2017). “Therapeutic effects of static magnetic field on wound healing in diabetic rats.” PMID: 28459073; DOI
Man, D., et al. (1999). “The influence of permanent magnetic field therapy on wound healing in suction lipectomy patients: A double-blind study.” PMID: 11149796
Morris, et al. (2007). “Chronic static magnetic field exposure alters microvessel enlargement resulting from surgical intervention.” PMID: 17478604; DOI
Morris, et al. (2008). “Acute exposure to a moderate strength static magnetic field reduces edema formation in rats.” PMID: 17982018; DOI
Rosen, A.D. (2003). “Mechanism of action of moderate-intensity static magnetic fields on biological systems.” PMID: 14515021
Shen, J.G., et al. (2009). “Effect of static magnetic field on deep wound healing of SD rats.” PMID: 19522401
Weintraub, M.I., et al. (2003). “Static magnetic field therapy for symptomatic diabetic neuropathy: A randomized, double-blind, placebo-controlled trial.” PMID: 12736891; DOI









